
Elizabet Paunović, Head of World Health Organization (WHO)’s European Center for Environment and Health, explains in an interview for the Balkan Green Energy News how air pollution is responsible for various diseases and hundreds of thousands of premature deaths in Europe. Paunović says that WHO’s focus in the region, apart from the air quality, is on water and sanitation and contamination sites. While stressing the importance of strengthening regional cooperation towards environmental safety, she also announces a new project to start in Serbia for safe management of contaminated sites to prevent negative impact on human health and the environment.
In your opinion, do the Western Balkans countries pay enough attention to the environmental protection from the health point of view? Are they aware of the need to improve environmental protection in order to protect health?
Each year, at least 1.4 million Europeans still die prematurely as a consequence of polluted environments. The burden of environmental health issues still amounts to at least 15% of Europe’s total deaths.
Air pollution is the single largest environmental health risk in Europe. WHO estimates that every year, ambient (outdoor) air pollution causes nearly 500 000 premature deaths; household (indoor) air pollution from solid-fuel combustion for heating and cooking is responsible for nearly 120 000 premature deaths. Unfortunately, some of our Member States in the Balkans and south-eastern Europe are worst in region for air quality, but they are aware of the need to improve and we are working extensively in the Region on this topic.
Another issue is historical industrial contamination and polluted sites that still require remediation. Contamination can affect soil, air, food and drinking water, and people can be exposed directly through ingestion, inhalation, skin contact, and dermal absorption to a host of noxious chemical agents. About one quarter of approximately 350 000 known contaminated sites in EEA countries are due to waste or hazardous waste. Various studies estimate that approximately 2–6% of the population in the WHO European Region are affected by waste-related exposures. Actions in respect to these problems are also needed in the SEE region.
What steps they must take to organize themselves better regarding this? Have they started to apply a multisectoral approach and developed much needed monitoring and data collection mechanisms?
The need for coordinated action on environment and health issues remains clear. Most WHO Member States in south-eastern Europe are either in the EU or accession countries. They need to strengthen monitoring of the health impacts to influence sectoral policies that protect their populations. One example would be in the energy policy and the use of coal. This naturally negatively affects air quality with an impact on health as I already explained. Subsidy policies and affordability linked with the high costs of other healthier and greener sources, causes that the coal is widely used in SEE region for household uses, for heating and cooking. This also plays a role: while deaths from ambient air pollution occur in all European countries, regardless of their income level, those from household air pollution are over five times greater in low- and middle-income countries than in wealthier ones.
Another important factor to consider is the cross-border implications of pollution of natural resources such as water and air. Two large international conventions that work to tackle this problem are the Convention on Long-range Transboundary Air Pollution and the Convention on the Protection and Use of Transboundary Watercourses and International Lakes, of which the Protocol on Water and Health is a component of the latter. WHO coordinates the work of the Joint Task Force on the Health Aspects of Air Pollution which provides evidence of the health effects and promotes use of the Convention’s instruments to address these effects. For the Protocol on Water and Health, the WHO Regional Office for Europe and the United Nations Economic Commission for Europe (UNECE) provide the joint secretariat to the Protocol and coordinate activities for its implementation.
Recently adopted as the outcome of the Sixth Ministerial Conference on Environment and Health provides Ostrava Ministerial Declaration on Environment and Health additional framework for intersectoral actions. All WHO European Member States committed themselves to develop National portfolios for action on environment and health by the end of 2018. Development of these portfolios is an excellent opportunity for boosting coordinated intersectoral actions.
You have recently said that 5,400 people die in Serbia annually due to diseases associated with air pollution, and that there is a gap between rural and urban areas when it comes to the quality of water. In this regard, where Serbia and other countries in the region stand in comparison to the developed European countries?
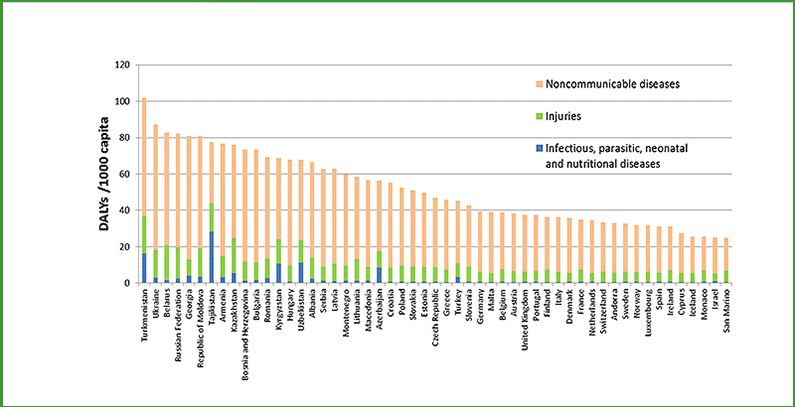
It’s easiest to illustrate that with the following chart, showing the proportion of environment-related disability-adjusted life years (DALYs) per capita in Europe. As you can see, non-communicable diseases are the largest component for pretty much all our Member States, but there are definitely inequalities evident across the Region. A share of DALY’s caused by environmental factor, and as I pointed out by the air pollution as the single biggest environmental cause of diseases and premature deaths is contributing to this figure.
We have a strong history of working with Serbia to improve the situation. For example, in May 2014 there was widespread flooding in the Balkans affecting Bosnia and Herzegovina, Croatia and Serbia. Learning from the experiences of that event there has been a need to shift the emphasis from disaster response to long-term risk management. Small-scale drinking-water systems in rural areas of Serbia are particularly challenged by such events. Registered water-related outbreaks in the past decade were mostly attributed to small-scale water supplies, indicating that these systems represent a potential health risk. A national-level systematic survey was undertaken in 2016 to gain better insight on how the aforementioned particularities and challenges of small-scale systems may affect the quality of drinking-water supplied to rural populations. The findings clearly showed a significant urban-rural gap in water-quality. About one third of all small supplies showed faecal contamination; 71% of piped systems and 77% of individual supplies in rural areas were found to require improvement action. Since its publication, the survey has induced policy actions and measures for the improvement of rural water supplies in Serbia, in particular proposing a new provision for implementation of the water safety plan approach in the draft law on water intended for human consumption and improving enforcement of regulation on the foundation and ownership of water supply systems.
Is it possible to establish direct and reliable link between premature deaths and air pollution, since its influence spans through the years and is not so visible in relation to many other factors?
Yes, air pollution can affect our health in many ways with both long and short term effects. New data has revealed a stronger link between both indoor and outdoor air pollution exposure and cardiovascular diseases, such as strokes and ischaemic heart disease, as well as between air pollution and cancer. This is in addition to air pollution’s role in the development of respiratory diseases, including acute respiratory infections and chronic obstructive pulmonary diseases.
Furthermore, the International Agency for Research on Cancer has classified air pollution in general, as well as particulate matter as a separate component of air pollution mixtures, as carcinogenic.
Different groups of individuals are affected by air pollution in different ways. More severe health impacts are seen among those people who are already ill. In addition, more vulnerable populations like children, the elderly and those households with lower incomes and limited access to health care are more susceptible to the adverse effects from exposure to air pollution.
In addition to improving the water and air quality, what other key environmental issue needs to be addressed in Serbia and the region in the context of health?
As already mentioned, the other major environmental issues continue to be improving climate resilience, especially in regard to heat-waves and flooding, remediation of industrial contaminated sites, and improved waste-water treatment.
What is the impact of climate change on health in Europe and the Western Balkans? Have there been emerging any new illnesses which are not typical for this climate? Have you been in contact with the governments of the Western Balkans countries and what steps have been taken in this regard?
The current and potential climate-related health risks include direct effects that mostly occur through changes in extreme weather events, and indirect effects that are mainly induced by changes in major environment, social and economic determinants. There are three main areas of public health concern related to climate change: extreme weather, changing infectious diseases and impacts on air quality, food and water safety and security.
Extreme weather, such as heat-waves, cold-spells, storms, floods, droughts and fires are increasing in frequency, intensity and duration, endangering fundamental health determinants and increasing threats of injuries, communicable and non-communicable diseases, stress-related mental illness and infrastructural damage.
Changing infectious diseases, such as vector-borne, food and water-borne, as well as respiratory diseases are changing in temporal and geographical distribution due to changing climate. Climate change is projected to lead to the spreading and increase of disease vectors including, the castor bean tick, mosquitos some species of sandflies.
Air quality, food and water security are three determinants of human health and well-being that are significantly altered by long-term changes of local and global climates as well as by sudden extreme weather events.
By affecting the social factors underlying sustainable development (poverty, food, employment, income and livelihood, gender, education, housing) both directly or indirectly, climate change is expected to cause large human migrations, temporary and permanent; sudden and planned, some of which we have already witnessed in parts of the world.
What is the WHO focus in the region when it comes to the environmental impact on the health? What projects do you implement? What are the further plans?
In our office, the WHO European Centre for Environment and Health in Bonn, Germany, the main areas of our work are water and climate, living and working environments, and environment and health impact assessment. These activities are contributing to the development of healthy and safe environments that support resilient and inclusive communities across our Region. Within this scope, we work on a large spectrum of technical areas, some of which we have already talked about, but also including chemical safety, environmental noise, workers’ health protection, amongst others.
As mentioned, particular focus areas in south-eastern Europe continue to be air quality, water and sanitation and contaminated sites. Indeed, we are just about to start a new project in Serbia on strengthening national capacities and inter-sectorial synergies for safe management of contaminated sites and related hazardous substances to prevent negative impact on human health and the environment, within the scope of the Strategic Approach to International Chemicals Management (SAICM) policy framework.
I am confident that with continued collaboration with the WHO Regional Office for Europe, as well as strengthened international cooperation in the region, we will achieve our vision of safe and supportive living and working environments that both protect and promote health and well-being.



